New York maternal medical negligence claims must be filed within 2.5 years under CPLR §214-a, with no infancy toll because the mother is the adult patient. Public-hospital cases require a 90-day Notice of Claim under GML §50-e. When maternal injury results in death, EPTL §5-4.1 imposes a separate two-year wrongful death deadline. Per the CDC NCHS Health E-Stats Maternal Mortality Report (March 2026), the U.S. maternal mortality rate was 17.9 deaths per 100,000 live births in 2024 (649 deaths), with profound racial disparities — Black women experienced 44.8 deaths per 100,000 in 2024, more than three times the rate for White women. The leading causes of pregnancy-related deaths are hemorrhage, infection/sepsis, thrombotic embolism, and cardiovascular conditions, which together account for the majority of preventable maternal deaths. Porter Law Group represents New York mothers and their families in cases of maternal medical negligence — when the obstetric, anesthesia, or hospital team failed to recognize or treat a maternal complication that produced injury or death.
Settlement
Jury Verdict
Settlement
Settlement
Maternal negligence cases differ fundamentally from infant birth injury cases. The patient is the adult mother, not the child — which means the CPLR §208 infancy toll does not apply, and the strict 2.5-year statute under CPLR §214-a runs from the date of malpractice. Mothers who suffered postpartum hemorrhage, hypertensive emergencies, infection/sepsis, anesthesia complications, or other obstetric injuries face a much shorter window than parents pursuing claims on behalf of an injured child. This timing pressure is the single most important reason to consult an experienced maternal negligence attorney promptly.
Porter Law Group has recovered more than $500 million for seriously injured clients since 2009. Led by Harvard-educated attorney Michael S. Porter, a former U.S. Army JAG Corps Captain with over 20 years of trial experience, the firm retains maternal-fetal medicine specialists, anesthesiologists, critical care physicians, and life care planners on every case. Seven of eight partner-level attorneys are recognized by Super Lawyers, a distinction earned by fewer than 5% of New York attorneys.
"Maternal cases are timing-sensitive in ways that infant cases are not. The mother is the adult patient, so the statute runs against her — not against the child. When a mother suffered preventable postpartum hemorrhage or eclampsia and is still recovering from the trauma, the family often does not realize the clock is already running. Two and a half years moves faster than people think."
— Michael S. Porter, J.D., Porter Law Group

REQUEST A NO-OBLIGATION CASE REVIEW
Maternal medical negligence is medical malpractice where the mother is the patient who suffered the injury — distinct from birth injury cases where the child is the injured patient. The legal framework follows New York's traditional four-element medical malpractice structure:
| Element | What Plaintiff Must Prove in a Maternal Negligence Case |
| Duty | Provider had a doctor-patient or hospital-patient relationship with the mother |
| Breach | The team failed to recognize or respond to a maternal complication in the manner required by accepted standards (typically established by reference to peer-reviewed obstetric literature, ACOG Practice Bulletins and Committee Opinions, the 2024 ACOG Clinical Practice Guideline on First and Second Stage Labor Management, and the AAP/ACOG Guidelines for Perinatal Care) |
| Causation | The failure was a substantial factor in producing the maternal injury (NY's substantial factor causation standard) |
| Damages | Documented physical, cognitive, reproductive, psychological, or economic injury to the mother |
The most important practical distinction from child-centered birth injury claims: the mother is an adult, so the infancy toll does not apply, and the statute is much shorter. Maternal claims must move quickly.
The United States has the highest maternal mortality rate among high-income countries, and the trend lines tell a serious story. Per the CDC NCHS Health E-Stats Report on Maternal Mortality 2024 (published March 2026) and the CDC NCHS Health E-Stats Report on Maternal Mortality 2023 (published February 2025):
| Year | U.S. Maternal Mortality Rate (per 100,000 live births) | Total Maternal Deaths |
| 2022 | 22.3 | 817 |
| 2023 | 18.6 | 669 |
| 2024 | 17.9 | 649 |
The 2024 rate represents a slight decrease from 2023 that the CDC notes is not statistically significant. The downward trend from the 2022 peak reflects partial recovery from the pandemic-era spike but the U.S. rate remains elevated relative to other high-income countries.
Racial disparities are profound. Per the same CDC source, in 2024:
Per the 2025 March of Dimes Report Card (citing 2019-2023 averages), American Indian/Alaska Native women experienced 60.8 deaths per 100,000 live births, the highest rate of any racial/ethnic group, followed by Non-Hispanic Black women at 53.7 per 100,000 and Native Hawaiian/Pacific Islander women at 40.7 per 100,000.
Age disparities are also significant. Per the CDC 2024 maternal mortality report, the maternal mortality rate for women age 40 and older was 62.3 deaths per 100,000 live births in 2024 — five times higher than for women younger than age 25 (13.7 per 100,000).
The CDC defines a maternal death using the WHO definition: "the death of a woman while pregnant or within 42 days of termination of pregnancy, irrespective of the duration and the site of the pregnancy, from any cause related to or aggravated by the pregnancy or its management, but not from accidental or incidental causes." Maternal deaths are coded under ICD-10 codes A34, O00–O95, and O98–O99.
Per the CDC Pregnancy-Related Mortality Surveillance (citing 2023 data) and consistent peer-reviewed obstetric literature, the leading causes of pregnancy-related deaths are:
| Cause | Recognized Mechanism | Primary Source |
| Hemorrhage | Uterine atony, retained placenta, lacerations, coagulopathy | ACOG Practice Bulletin No. 183 (October 2017, Obstetrics & Gynecology 130(4):e168-e186) |
| Infection/sepsis | Chorioamnionitis, postpartum endometritis, surgical site infection | ACOG Committee Opinion No. 712 (August 2017) |
| Thrombotic embolism | Pulmonary embolism, amniotic fluid embolism | Peer-reviewed obstetric literature |
| Cardiovascular conditions | Cardiomyopathy, ischemic heart disease, hypertensive heart disease — accounts for >1/3 of pregnancy-related deaths per CDC | CDC Pregnancy-Related Mortality Surveillance |
| Hypertensive disorders | Preeclampsia, eclampsia, HELLP syndrome | Preeclampsia practice page |
| Anesthesia complications | Failed intubation, aspiration, neuraxial complications | Peer-reviewed obstetric anesthesia literature |
Each of these causes has well-established recognition standards and management protocols. When the team fails to recognize or treat the condition in accordance with these standards and the mother is injured or dies, the failure may be actionable as medical negligence.
U.S.-specific note: Per CDC Pregnancy-Related Mortality Surveillance, cardiovascular conditions account for more than one-third of pregnancy-related deaths in the United States — making cardiovascular conditions the largest single category in U.S. data, even though hemorrhage remains the leading cause of maternal mortality worldwide per ACOG Practice Bulletin No. 183. The leading-causes list above presents the recognized causes by clinical category rather than by U.S.-specific frequency.
Per ACOG Practice Bulletin No. 183: Postpartum Hemorrhage (October 2017, Obstetrics & Gynecology 130(4):e168-e186), postpartum hemorrhage is defined as cumulative blood loss greater than or equal to 1,000 mL OR blood loss accompanied by signs or symptoms of hypovolemia within 24 hours after the birth process. The same Practice Bulletin notes that "maternal hemorrhage remains the leading cause of maternal mortality worldwide" and provides the canonical management algorithm.
ACOG Practice Bulletin No. 183 specifies a structured approach:
Active management of the third stage of labor to reduce postpartum hemorrhage incidence: oxytocin administration, uterine massage, and umbilical cord traction.
First-line treatment for hemorrhage from uterine atony (the most common cause): uterotonics — agents that contract the uterus.
Escalation when uterotonics fail: intrauterine balloon tamponade, tranexamic acid, surgical interventions including B-Lynch sutures, uterine artery ligation, and — if necessary to preserve the mother's life — peripartum hysterectomy.
The 2025 ACOG Clinical Practice Update: Use of Nonsurgical Hemorrhage-Control Devices provides additional revised guidance specifically on nonsurgical devices for postpartum hemorrhage management.
When the chart shows the team failed to recognize blood loss reaching the 1,000 mL threshold, failed to escalate care when uterotonics did not control bleeding, or failed to implement a documented institutional postpartum hemorrhage protocol, the case for malpractice may be strong. Per ACOG Practice Bulletin No. 183, "hemorrhage that leads to blood transfusion is the leading cause of severe maternal morbidity in the United States."
Six recurring failure patterns produce most maternal medical negligence claims in New York:
Failure 1 — Failure to recognize or treat postpartum hemorrhage. Per ACOG Practice Bulletin No. 183, postpartum hemorrhage requires real-time recognition and structured escalation. Failure to monitor blood loss accurately, failure to initiate uterotonics promptly, failure to escalate when bleeding is uncontrolled, and failure to implement institutional postpartum hemorrhage protocols are core negligence patterns.
Failure 2 — Failure to recognize or treat hypertensive emergencies. Severe-range blood pressure (≥160/110) requires treatment within 30 to 60 minutes per consistent peer-reviewed obstetric literature on preeclampsia management. Failure to administer antihypertensives, failure to administer magnesium sulfate for seizure prophylaxis, and failure to expedite delivery when severe features develop are core negligence patterns. See our Preeclampsia practice page for detail.
Failure 3 — Failure to recognize or treat sepsis. Maternal sepsis from chorioamnionitis, endometritis, or surgical site infection requires rapid recognition and broad-spectrum antibiotics. Per ACOG Committee Opinion No. 712: Intrapartum Management of Intraamniotic Infection (August 2017, Obstetrics & Gynecology 130:e95-e101), suspected intraamniotic infection should be treated with broad-spectrum antibiotics.
Failure 4 — Anesthesia complications. Failed intubation, aspiration, hypotension, high spinal block, local anesthetic systemic toxicity, and post-dural puncture headache are recognized obstetric anesthesia complications. Failure to follow ASA difficult airway algorithms, failure to recognize developing hypotension, or failure to manage anesthesia-related complications can be actionable.
Failure 5 — Failure to manage maternal cardiovascular conditions. Cardiovascular conditions account for more than one-third of pregnancy-related deaths per CDC data. Peripartum cardiomyopathy, pulmonary edema, and cardiac arrhythmias require recognition and prompt management — often by a multidisciplinary team including maternal-fetal medicine and cardiology.
Failure 6 — Failure to manage Pitocin/oxytocin leading to maternal injury. Pitocin-induced uterine hyperstimulation can cause uterine rupture (particularly in VBAC), placental abruption, postpartum hemorrhage, and cervical or vaginal lacerations. Maternal injury from Pitocin misuse is a recognized basis for negligence.
New York places no statutory cap on damages in medical malpractice cases. The pending NY S1608 (2025-2026) Borrello-sponsored bill proposing a $250,000 cap on noneconomic damages remains pending before the Senate Judiciary Committee and has not been enacted. Recoverable damages in maternal negligence cases include:
Past and future medical expenses for the maternal injury — including hospitalization, surgery, intensive care, rehabilitation, mental health treatment for postpartum trauma, and any ongoing medical needs.
Lost wages and lost earning capacity when the maternal injury impairs the mother's ability to work. This category can be substantial when the mother required hysterectomy, suffered permanent disability, or developed long-term sequelae such as Sheehan syndrome (pituitary necrosis from hemorrhagic shock).
Pain and suffering damages are not capped in New York. Maternal cases often involve substantial pain and suffering damages because of the traumatic nature of the injuries — emergency hysterectomy, near-death from hemorrhage, eclamptic seizures, ICU admission, extended NICU separation from the newborn.
Loss of reproductive capacity. Cases involving emergency hysterectomy or other loss of fertility produce substantial damages because of the permanence of the loss — particularly for younger mothers.
Loss of consortium. The mother's spouse may pursue a separate loss of consortium claim, also subject to a 2.5-year statute under CPLR §214-a.
Wrongful death. When maternal medical negligence results in the mother's death, the surviving spouse and dependents may pursue a wrongful death claim under EPTL §5-4.1 within two years of death. Wrongful death damages include pecuniary losses to the spouse and dependents, loss of parental nurture and guidance for surviving children, and conscious pain and suffering of the decedent before death.
FIND OUT WHAT YOUR MATERNAL NEGLIGENCE CASE IS WORTH →
Porter Law Group's published catastrophic case results include three pediatric birth injury settlements that demonstrate the firm's track record in complex obstetric injury cases. View all case results →
$8,300,000 Settlement: A premature infant suffered profound permanent disabilities, including cerebral palsy, after physicians failed to properly manage the mother's pre-gestational diabetes. The structured settlement provides lifetime care and therapy funding.
$8,250,000 Settlement: An infant sustained permanent physical and cognitive disabilities after delayed response to fetal distress during labor.
$8,120,000 Settlement: An infant suffered permanent delivery-related injuries caused by mismanaged labor and delivery.
Every case is different. Past results do not guarantee future outcomes.
Maternal negligence claims have shorter deadlines than birth injury claims because the mother is an adult and the infancy toll does not apply.
| Category of Defendant | Statute of Limitations | Infancy Toll Applies? | Effective Deadline | Primary Statute |
| Private hospital / private physician | 2.5 years | No — patient is adult mother | 2.5 years from malpractice | CPLR §214-a |
| Public hospital (NYC Health + Hospitals, SUNY Upstate, SUNY Downstate, Stony Brook, county hospitals) | 1 year and 90 days after Notice of Claim | No | 90 days from injury to file Notice of Claim | GML §50-e |
| Wrongful death (mother) | 2 years from date of death | N/A | 2 years from death | EPTL §5-4.1 |
| Continuous treatment | 2.5 years from last treatment for same condition | N/A | Last treatment + 2.5 years | CPLR §214-a |
The infancy toll of CPLR §208 — which extends most birth injury deadlines to the child's 10th birthday — does not apply to maternal claims because the mother is an adult patient. This is the single most important timing distinction in maternal negligence cases.
ACT NOW BEFORE YOUR MATERNAL NEGLIGENCE DEADLINE EXPIRES →
Looking for Medical Compensation after a Dog Attack?
Let us help. Our clients don't have to pay anything unless we win.
1. Request the complete labor-and-delivery, postpartum, and hospital records. Under Public Health Law §18, you are entitled to your complete medical records within a reasonable time of a written request. Critical documents include the labor-and-delivery records, the operative note (for cesarean cases), the anesthesia record, the postpartum nursing flowsheet, blood loss documentation, vital signs throughout admission, lab values, and any rapid response or code blue records.
2. Document the timeline of events. Reconstruct what happened from your own memory while it is fresh, then compare against the medical records. Note when complications were first apparent, when interventions were initiated, when you reported symptoms, and how the team responded.
3. Document ongoing physical and psychological injury. Keep a dated log of symptoms, medical visits, mental health treatment, and impact on daily activities. Postpartum trauma, PTSD, anxiety, and depression are recognized injuries in maternal negligence cases.
4. Preserve all imaging, pathology, and lab results. Request complete copies of any imaging studies, pathology reports, and lab values from your hospitalization.
5. Act immediately if you delivered at a public hospital. The 90-day Notice of Claim deadline under GML §50-e is unforgiving. Mothers who delivered at NYC Health + Hospitals, SUNY Upstate, SUNY Downstate, Stony Brook, or county hospitals must file Notice of Claim within 90 days.
6. Recognize the timing pressure. Unlike infant birth injury claims that may have until the child's 10th birthday under the infancy toll, maternal claims run on the adult statute — 2.5 years from malpractice, with no extension. Consult an attorney as soon as you have reason to suspect negligence.
7. Consult a New York maternal medical negligence attorney promptly. Porter Law Group offers free consultations on a contingency-fee basis and handles every stage of the case.
GET A FREE CASE REVIEW: CALL (833) PORTER-9 →
Porter Law Group represents mothers and their families in maternal medical negligence cases throughout New York State, with a statewide practice reaching every county and jurisdiction. Our Syracuse headquarters serves Central and Upstate New York, while attorneys travel regularly to downstate courthouses for cases in the five boroughs, Westchester, and Long Island.
Serving Clients statewide, including Maternal Medical Negligence Attorney in Syracuse, New York City, Manhattan, Buffalo, Rochester, Albany, Yonkers, White Plains, Utica, Binghamton, Long Island (Nassau and Suffolk Counties), Saratoga Springs, Ithaca.
Wherever you were injured in New York, call (833) PORTER-9 for a free consultation with an experienced maternal medical negligence attorney.
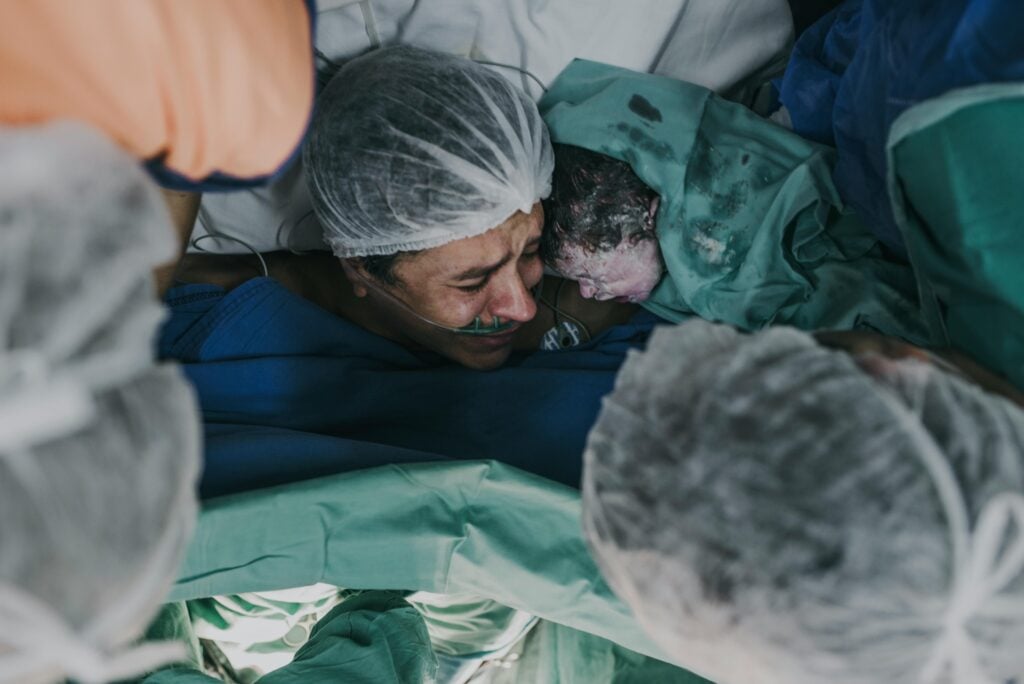
Maternal medical negligence and birth injury are related but legally distinct. Maternal medical negligence cases involve injury to the mother — postpartum hemorrhage, hypertensive emergencies, sepsis, anesthesia complications, cardiovascular events, or maternal death. The patient is the adult mother. Birth injury cases involve injury to the child —HIE, cerebral palsy, brachial plexus injury, or other injuries to the newborn. The patient is the child. The most important practical difference is the statute of limitations: birth injury claims (the child's claim) are tolled by CPLR §208 until the child's 10th birthday; maternal claims (the mother's claim) follow the adult 2.5-year statute under CPLR §214-a with no infancy toll. Many catastrophic obstetric cases involve both — maternal injury plus child injury — and each must be analyzed separately under its own statute.
Maternal negligence claims must be filed within 2.5 years from the date of malpractice under CPLR §214-a. The infancy toll of CPLR §208 does not apply because the patient is the adult mother. Deliveries at public hospitals (NYC Health + Hospitals, SUNY Upstate, SUNY Downstate) require a Notice of Claim within 90 days of the injury under General Municipal Law §50-e. When maternal injury results in death, EPTL §5-4.1 imposes a separate 2-year wrongful death deadline. The continuous treatment doctrine may toll the 2.5-year deadline when the same provider continues treating the mother for the same condition that caused the injury, but this is fact-specific and does not extend the deadline indefinitely.
Per the CDC NCHS Health E-Stats Report on Maternal Mortality 2024 (March 2026), the U.S. maternal mortality rate was 17.9 deaths per 100,000 live births in 2024 (649 maternal deaths) — a slight but not statistically significant decrease from 18.6 in 2023 and 22.3 in 2022. The U.S. rate is the highest among high-income countries and demonstrates profound racial disparities: Black women experienced 44.8 deaths per 100,000 in 2024, more than three times the rate for White women (14.2 per 100,000), with Hispanic women experiencing a significantly lower rate. Per the 2025 March of Dimes Report Card, American Indian/Alaska Native women had the highest rate among racial/ethnic groups at 60.8 per 100,000. The maternal mortality rate for women age 40 and older was 62.3 per 100,000 — five times higher than for women under 25.
Per ACOG Practice Bulletin No. 183: Postpartum Hemorrhage (October 2017, Obstetrics & Gynecology 130(4):e168-e186), postpartum hemorrhage is defined as cumulative blood loss greater than or equal to 1,000 mL OR blood loss accompanied by signs or symptoms of hypovolemia within 24 hours after the birth process. ACOG specifies a structured management approach: active management of the third stage of labor (oxytocin, uterine massage, cord traction); first-line uterotonics for hemorrhage from atony; escalation to intrauterine balloon tamponade, tranexamic acid, surgical interventions, or peripartum hysterectomy when uterotonics fail. When the chart shows the team failed to recognize blood loss reaching the 1,000 mL threshold, failed to escalate care when uterotonics did not control bleeding, or failed to implement a documented institutional postpartum hemorrhage protocol, the case for malpractice may be strong. Per the same Practice Bulletin, "hemorrhage that leads to blood transfusion is the leading cause of severe maternal morbidity in the United States."
Per CDC Pregnancy-Related Mortality Surveillance (citing 2023 data), the leading causes of pregnancy-related deaths are hemorrhage, infection or sepsis, and thrombotic pulmonary or other embolisms. Cardiovascular conditions account for more than one-third of pregnancy-related deaths per CDC data — including peripartum cardiomyopathy, ischemic heart disease, and hypertensive heart disease. Hypertensive disorders of pregnancy (preeclampsia, eclampsia, HELLP syndrome) and anesthesia complications also contribute substantially. Each of these causes has well-established recognition standards and management protocols documented in ACOG Practice Bulletins, Committee Opinions, and Clinical Practice Guidelines. When the team fails to recognize or treat the condition in accordance with these standards and the mother is injured or dies, the failure may be actionable as medical negligence.
Yes, and the disparities are profound and well-documented. Per the CDC NCHS Health E-Stats Report on Maternal Mortality 2024, Black women experienced 44.8 maternal deaths per 100,000 live births in 2024, compared to 14.2 for White women — more than three times the rate. Per the 2025 March of Dimes Report Card citing 2019-2023 averages, American Indian/Alaska Native women experienced 60.8 deaths per 100,000 — the highest rate of any racial/ethnic group. Native Hawaiian and Pacific Islander women experienced 40.7 per 100,000. These disparities reflect complex contributors including unequal access to high-quality maternal care, implicit bias in clinical decision-making, differential rates of underlying medical conditions, and structural inequities in healthcare delivery. From a malpractice perspective, the disparities matter analytically because care that meets the standard for one patient may be inadequate when delivered to a higher-risk patient — and patterns of differential recognition or response can support liability when injury results.
The single most important timing distinction in maternal negligence is the non-applicability of the infancy toll. Birth injury claims (the child's claim) are tolled by CPLR §208 until the child's 10th birthday, giving families substantial time to recognize developmental sequelae and consult an attorney. Maternal claims (the mother's claim) follow the adult 2.5-year statute under CPLR §214-a with no extension. Mothers who suffered postpartum hemorrhage, eclampsia, sepsis, or other obstetric injuries often spend the first months recovering physically and psychologically — by the time families consider whether the care was negligent, substantial portions of the 2.5-year window may have elapsed. Public-hospital cases face an even tighter window: 90 days from the injury to file Notice of Claim under GML §50-e, with motions for leave to serve a late notice of claim under GML §50-e(5) requiring discretionary judicial relief that is never guaranteed.
Many catastrophic obstetric cases involve both maternal injury and child injury arising from the same negligent care. For example, undertreated severe preeclampsia can produce both maternal eclamptic seizures and fetal injury from placental insufficiency; mismanage shoulder dystocia can produce maternal lacerations and infant brachial plexus injury; Pitocin misuse can produce maternal uterine rupture and infant hypoxic injury. From a legal perspective, the maternal claim and the child's claim are separate and each runs on its own statute. The mother's claim runs on the adult 2.5-year statute under CPLR §214-a without infancy toll; the child's claim runs on the same 2.5-year statute but with the CPLR §208 infancy toll capped at the 10th birthday. Coordinated representation of both the mother and the child by experienced maternal-fetal-medicine and birth-injury counsel is critical — Porter Law Group routinely represents both mother and child in cases involving combined maternal and infant injury.

Michael S. Porter is the founder and managing partner of Porter Law Group, representing New York families in birth injury, medical malpractice, and catastrophic injury cases. A graduate of Harvard University (B.A., 1994) and Syracuse University College of Law (J.D., 1997), Porter served four years as a Captain in the U.S. Army Judge Advocate General's Corps. Selected to Super Lawyers for 14 consecutive years (2012–2025), he holds a 10.0 Superb rating on Avvo and a Distinguished rating from Martindale-Hubbell.
Bar Admissions: New York State Bar | U.S. District Court, Northern and Western Districts of New York
Memberships: New York State Bar Association, Onondaga County Bar Association, New York State Academy of Trial Lawyers, Multi-Million Dollar Advocates Forum
If you suffered injury during pregnancy, labor, delivery, or the postpartum period in New York due to medical negligence, critical deadlines may run faster than you expect. The infancy toll does not apply to your claim because you are the adult patient — your 2.5-year statute under CPLR §214-a runs from the date of malpractice. Public-hospital cases require a Notice of Claim within 90 days. Wrongful death claims follow a separate 2-year deadline under EPTL §5-4.1.
Contact Porter Law Group today at (833) PORTER-9 for a free, no-obligation consultation. We operate on a contingency-fee basis under Judiciary Law §474-a, so you pay nothing unless you win.
Phone: +1 833-767-8379
Email: info@porterlawteam.com
Monday to Friday: 8 AM to 5 PM | Saturday and Sunday: Closed

Avoid sharing confidential information via contact form, text, or voicemail as they are not secure. Please be aware that using any of these communication methods does not establish an attorney-client relationship. *By appointment only.
The information contained on this site is proprietary and protected. Any unauthorized or illegal use, copying, or dissemination will be prosecuted to the fullest extent of the law. All content on this site is provided for informational purposes only. It is not, nor should it be taken as medical or legal advice. None of the content on this site is intended to substitute for medical advice, diagnosis, or treatment. Attorney Advertising.
We serve clients in every city and county in New York State. These include places like: The Adirondacks, Albany, Alexandria Bay, Amsterdam, Astoria, Auburn, Ballston Spa, Batavia, Beacon, Binghamton, Brooklyn, Buffalo, Canandaigua, Carthage, Cattaraugus, Catskill, Cayuga Lake, Cazenovia, Chelsea, Clayton, Clifton Park, Cobleskill, Colonie, Cooperstown, Corning, Cortland, Delhi, Delmar, Dunkirk, East Aurora, East Hampton, Elmira, Fayetteville, Finger Lakes, Flushing, Fredonia, Fulton, Garden City, Geneva, Glen Cove, Glens Falls, Gloversville, Gouverneur, Great Neck, Greenwich Village, Hamilton, Hammondsport, Harlem, Haverstraw, Hempstead, Herkimer, Hornell, Hudson, Huntington, Ilion, Ithaca, Jamaica, Jamestown, Johnstown, Kingston, Lake George, Lake Placid, Lewiston, Little Falls, Liverpool, Lockport, Long Island City, Lowville, Malone, Manhattan, Manlius, Massena, Medina, Middletown, Monticello, Montauk, Mount Vernon, New Paltz, New Rochelle, Newburgh, Niagara Falls, North Tonawanda, Norwich, Nyack, Ogdensburg, Old Forge, Olean, Oneida, Oneonta, Ossining, Oswego, Penn Yan, Peekskill, Plattsburgh, Port Chester, Potsdam, Poughkeepsie, Queens, Rhinebeck, Riverhead, Rochester, Rome, Rye, Sag Harbor, Saranac Lake, Saratoga Springs, Schenectady, Seneca Falls, Seneca Lake, Skaneateles, SoHo, Southampton, Spring Valley, Staten Island, Stony Brook, Suffern, Syracuse, Tarrytown, The Bronx, Thousand Islands, Ticonderoga, Troy, Tupper Lake, Utica, Warsaw, Waterloo, Watertown, Watkins Glen, Wellsville, White Plains, Williamsburg, Woodstock, Yonkers, and many more communities throughout New York State.
Copyright © 2026, Porter Law Group. Personal Injury Lawyers
Made with 💛 by Gold Penguin